What is Plantar Fasciitis?
When you take your first steps of the day, do you feel a stabbing pain in your heel? Or does your foot ache part way into a jog or run? That could be plantar fasciitis talking to you. Plantar fasciitis is the inflammation of the plantar fascia connective tissue (that big tendon on the bottom of your foot). It extends from your calcaneus bone (heel) to the phalanges (toes). This thick tissue is shaped like a bowstring that helps support the arch of the foot while also absorbing shock while walking.
When the plantar fascia is put under too much tension and stress and repeatedly stretched, it can cause minuscule tears that result in painful inflammation.
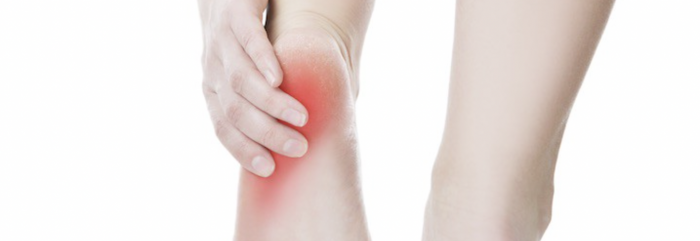
What causes Plantar Fasciitis?
Although there is no one clear cause for plantar fasciitis, a variety of risk factors can contribute to the onset of this painful condition and can happen to anyone. Plantar fasciitis is commonly seen in active and sedentary populations. So what gives?
If a person has a sedentary lifestyle in combination with being “overweight,” they are susceptible when the extra weight causes extra strain on plantar fascia while doing daily activities. Athletes on the other hand, may experience the same pain as a result from excessive running or being on their feet for prolonged periods of time. Of course people in between, that are mildly active and in the “appropriate” weight range for their height can also experience plantar fasciitis. Hurray.
Then there’s your foot’s biomechanics to consider. Individuals with flat feet / low arches (also called pes planus) and high arches (pes cavus), may play another major role in developing plantar fasciitis. Those with flat feet often experience over pronation of the foot which can result in excessive strain of the plantar fascia, while pes cavus foot types cannot dissipate force evenly due to limited range of motion in the joints, which results in decreased flexibility in the calf muscles and Achilles tendon.
What activities might cause plantar fasciitis? Should I avoid them?
Plantar fasciitis is quite common in runners, likely due to the accessibility of the activity amongst marathoners, weekend warriors and people just trying to get into it. It can also affect athletes whose sports require explosive power (i.e. gymnasts, basketball, tennis, dancers, etc.)
In runners, the loading force can be up to 200% of their body weight. With repetitive motion and increasing intensity during training, it can lead to overuse and result in pain and inflammation in the heel.
While avoiding the activity altogether to prevent getting plantar fasciitis isn’t recommended, we suggest starting any new activity slowly to allow your body’s joints, muscles and tendons to properly adapt over time.
How to manage plantar fasciitis
Depending on how severe the condition is in each individual (please see your doctor to make sure your diagnosis is correct and the pain / discomfort actually is plantar fasciitis and not something else like a bone fracture etc), there are both conservative and radical approaches to treating plantar fasciitis:
Conservative therapies may include:
- RICE method – Rest, Ice, Compression, Elevation. Although the focus is on Rest and Ice if you notice heat and swelling in the area.
- Taking analgesics as prescribed like Advil (ibuprofen) or Tylenol (acetaminophen) to relieve pain caused by plantar fasciitis accompanied with sufficient rest
- A physical therapist can use modalities to help speed the body’s natural healing process. They may have you work with a kinesiologist and prescribe a series of exercises or stretches that can strengthen the lower leg muscles and lengthen the Achilles tendon (see below for exercises)
- For those with pes planus foot types, foot orthotics can help to prevent overpronation of the foot, and help distribute forces more evenly
How can a kinesiologist help me with my plantar fasciitis?
Strengthening exercises are often recommended for muscles surrounding the ankle joint and supporting the foot, such as the tibialis anterior, tibialis posterior, and peroneal muscles, presumably to control pronation.
Again, depending on the root cause, if a client has pes cavus, the focus would be on stretching the calf to decrease muscle tightness. If someone has pes planus, focusing on strengthening the muscles in the arch of the foot take priority.
In both cases, since plantar fasciitis follows you around if you’re on your feet, and assuming you use your feet daily, we’d check that proper footwear or orthotics are a measure to support your foot while it heals. Not all people need to wear supportive footwear 24/7, especially if the issue can be corrected through exercise, stretches and time, however if you’re suffering from it now, and need to get your 8k run in tonight, no amount of stretching and strengthening this morning is going to help you during your run. Some individuals have been able to forgo use of orthotics and shoe insoles after time but this could depend on the root cause of the issue. Again, speak with your doctor about your options.
Exercises and stretches to help plantar fasciitis
- Heel raises: Stand on an elevated surface (stairs or step bench will work) with the ball of your foot, and put a rolled towel underneath your big toe joint. This puts your foot into a “toes-up” flexed position. Your heel should be elevated. As this isn’t a balance exercise, hold on to a banister or a stable structure, such as a chair or wall, for balance. Begin the heel raise with the concentric contraction by raising up for 3 seconds, holding the contraction for 2 seconds at the top. Lowering the heel towards the ground slowly (take another 3 seconds) and holding the stretched position for 3 seconds. Repeat this exercise for 8 – 12 repetitions, 3 sets a day. Start with two feet if your plantar fasciitis is quite acute and tender, then progress to one leg as your strength and comfort increases.
- Towel gathering: Seated on a chair with a towel laid flat in front of you, place your foot on top of the towel and using your toes, scrunch the towel towards you. Then, use your toes to push the towel away from you. To make this exercise more challenging, place a weighted object such as a soup can on the other end of the towel and repeat the exercise.
- Foot / calf stretch: Seated on a chair, place a rolled towel around the ball of your foot, and hold both ends of the towel in your hands. Gently pull on the towel so your foot flexes and pull your toes towards you, while also ensuring that the knee is straight. Hold this stretch for 15-30 seconds. For individuals who have a bit more flexibility and may find this exercise too easy, the exercise can be modified by using your hand to grab on to your toes, instead of using the towel. Without bending the knee, slowly lean forward until you feel your calf stretching.
If you’re suffering from plantar fasciitis, hopefully one of the above strategies sounds familiar as something your doctor or physio recommended for you, and remember to stick to the recommended regime for best results. If you’ve tried them but aren’t seeing any improvement, we strongly suggest checking back in with your physio or GP to rule out any other issues such as a fracture. In some cases where strengthening and stretching exercises aren’t making a difference, they may also refer you to a podiatrist for specialized help.
Co-Authored by Brian Lau